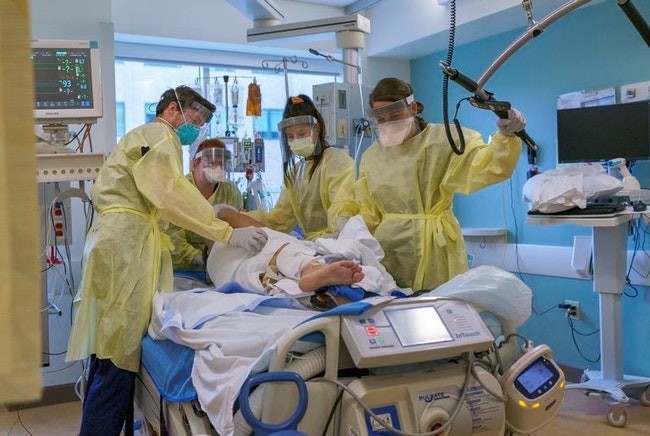
The intense care required for Covid-19 patients has exhausted nurses and other health care staff. (Oregon Health & Science University photo)
With the Covid-19 vaccine mandate looming, the Oregon Nurses Association stepped into the fray on Thursday, calling on the state to take “bold” action to give relief to nurses strained by exhausting shifts relief and to train a new corps.
In a news conference, association officials called on hospitals to allow nurses to take true work breaks, switch away from relying on temporary traveling nurses and step up investment in a wellness program to help nurses face mental health issues.
They also called for an increase in faculty salaries at Oregon colleges and universities to expand training for students, with loan forgiveness programs that would attract nurses to underserved areas.
“Nurses are calling for stakeholders, frontline workers and hospital executives to step up and reimagine how and why we provide health care,” said Lynda Pond, a registered nurse and president of the association’s board.
The association represents about 13,500 registered nurses out of nearly 72,000 licensed by the Oregon Board of Nursing.
The news conference comes amid a strike vote among 3,400 Kaiser Permanente Northwest nurses and other health professionals in Oregon over contract negotiations on pay and other issues. The nurses are represented by the Oregon Federation of Nurses and Health Professionals, which said that nationwide a majority of 52,000 Kaiser Permanente staff represented by 21 unions are currently voting on walkouts. In Oregon, the federation is expected to know the result of the vote on Monday. Before members walk off the job, the union has to give Kaiser Permanente a 10-day notice.
At Mid-Columbia Medical Center in The Dalles, nurses scheduled a rally Thursday evening. Their contract, negotiated by the Oregon Nurses Association, expired in June. And in another labor action, health care workers represented by Service Employees International Union Local 49 are holding a two-day strike that started Wednesday at McKenzie-Willamette Medical Center in Springfield over outsourcing, staffing standards and other issues.
In the meantime, all health care staff face an Oct. 18 vaccine mandate, which could reduce staffing throughout the state.
“We know that upwards of 90% of ONA members are vaccinated,” Pond said. “We also know that a small number of nurses across the state have made the decision to not get vaccinated, and those nurses will likely be terminated from their jobs.”
Only 83% of nurses are vaccinated, according to Oregon Health Authority data.
“We know that losing even a single nurse from the bedside will result in a greater strain on our health care system, and we have urged hospitals, and our lawmakers, to do everything they can to keep nurses working for the benefit of patients,” Pond said.
Next week, the Board of Nursing will consider a temporary rule that would make Covid-19 vaccination a requirement for obtaining a nursing license. The rule would not immediately affect licensed nurses, however.
“No nursing licenses will be revoked automatically on October 18 for noncompliance with the governor’s executive order,” said Barbara Holtry, spokeswoman for the nursing board.
She added that the board only investigates when it receives a complaint. Besides withdrawing a license, the board can impose a range of punishments, from a reprimand to a $5,000 fine.
The Oregon Health Authority has left it up to employers to police the mandate.
Scott Palmer, ONA spokesman, said that the temporary rule was just a housekeeping measure, adding that it “seems reasonable.”
Rather than discussing the mandate, Palmer said the association wanted to focus on the future.
Association board members blasted the hospital industry, accusing executives of putting their bottom line before staff well-being.
“The nurse staffing crisis didn’t start with Covid-19 or with vaccine mandates,” Pond said. “It’s been created and compounded by hospital executives who have consistently chosen to put profits ahead of patients.”
As a case in point, the association pointed a finger at Oregon Health & Science University.
“OHSU provides an example of what not to do in response to the ongoing crisis,” said Matt Calzia, a registered nurse and ONA nurse practice consultant.
In a September survey at OHSU, more than 90% of nurses reported feeling mentally exhausted in the past two months, nearly 80% said they were physically exhausted, 85% reported feeling overwhelmed and about 60% said they’d like to leave nursing.
Yet on Monday, OHSU notified its nursing staff that they may have to take a greater patient load at times in critical and acute care, Calzia said.
“Before this surge is even over, OHSU is already asking for nurses to go above and beyond yet again,” Calzia said.
OHSU’s communication staff did not respond by Thursday evening to a request for comment.
Nurses at OHSU traditionally have worked three 12-hour shifts a week, said Natasha Schwartz, an OHSU nurse and member of the association’s board. But she said that during the pandemic nurses have picked up extra shifts, working up to 60 hours a week.Often during a shift, nurses don’t get a break, officials said.
Calzia called on hospitals to end a “buddy break” system in which nurses fill in for each other during breaks by taking on more patients. He said hospitals need to have a dedicated set of fill-in nurses for breaks as provided for now at Sacred Heart Medical Center University District in Eugene and OHSU Health Hillsboro Medical Center.
“That is a simple fix to help with the fatigue,” Calzia said.
Another point of contention for the association is the use of contract nurses.
Calzia said that hospitals had become “dangerously dependent” on traveling nurses, which have been used to fill gaps in staffing, especially in southern Oregon where hospitals ran out of beds during the current surge. He said up to one-third of nurses in some hospitals are on contract and that some units are entirely staffed by so-called traveling personnel.
The Oregon Health Authority has signed contracts for $133 million with temporary staffing agencies to pay for dozens of contract nurses and other practitioners. The contracts include $12 million for Asante’s three hospitals in southern Oregon, $2 million for Providence Medford Medical Center and $2.5 million for Mercy Medical Center in Roseburg and $9 million for the Oregon State Hospital.
The health authority plans to bill the Federal Emergency Management Administration for the cost. Some of the contracts run through Dec. 31 and others expire Feb. 28.
The nurses association also urged hospitals and lawmakers to step up investment in mental health support. Calzia called on the Legislature to approve $1.8 million to add a mental health provision in the Oregon Wellness Program, which is funded by state and private dollars.
The Oregon Association of Hospitals and Health Systems did not respond directly to the association’s suggestions. Instead, it acknowledged in a statement that nurses are exhausted and said it has sounded the alarm about the workforce shortage.
“Hospitals have been doing whatever it takes to provide the best care and the best workplace possible as we continue to battle the pandemic,” the statement said. “We agree that this environment is unsustainable. Finding solutions that focus on the health of the communities we serve will take a high degree of trust and collaboration between stakeholders, the executive and legislative branches.”
Another major area for the association is the training of the next generation of nurses. Schwartz said faculty salaries need to be increased.
“Given the fact that nursing faculty can make significantly more in a clinical setting, we must address wage disparities to retain qualified educators,” Schwartz said.
She said students need more scholarships, too, and called for the creation of a nursing corps program which would forgive student loans. In exchange, graduates would work four years in areas with the worst shortages and in clinics that serve underserved and marginalized populations.
“Fixing the nursing pipeline will require partnerships, collaboration and innovative thinking,” Schwartz said. “Failing to address the nursing pipeline simply ensures an even greater crisis in our future.”
NEWS TIP? STORY IDEA? Please send an email to the Enterprise at [email protected].