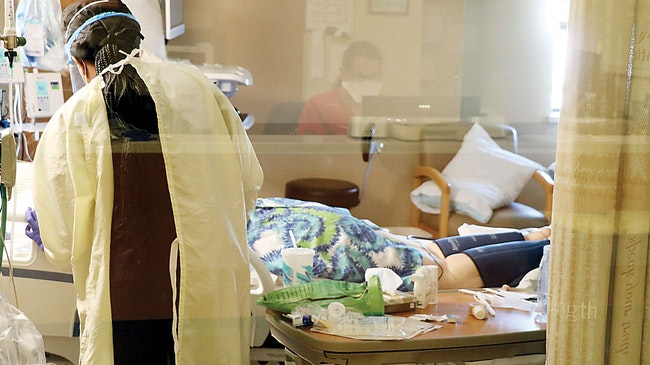
Registered nurse Dajanay Ash tends to a patient in intensive care in Saint Alphonsus Medical Center in Ontario. (Malheur Enterprise/LILIANA FRANKEL)
Getting hospitalized with Covid in an intensive care unit can result in a weeks-long ordeal, near-death experiences – and costs that range to six figures, according to health authorities and government officials.
No government agency has yet to report on what the total cost for intensive care treatment related to Covid has been in Oregon. A summer surge strained the state’s hospitals and at times more than 300 people were in intensive care, with more than 1,100 people otherwise ill enough with Covid to require hospitalization.
In the Boise region that includes Malheur County, over 95% of Covid patients in ICUs are unvaccinated, according to hospital representatives at St. Luke’s Health System, St. Alphonsus Health System and Valley Family Health Care. Health care experts have made it clear that the vast majority of severe cases are preventable with vaccination.
Covid patients on average stay in the ICU more than twice as long as other patients, costing millions of dollars.
The average cost of a Covid hospitalization requiring time in intensive care is $248,473 at Oregon Health & Science University in Portland, which takes the most severe cases from around the state.
That’s nearly three times more expensive than the average cost for non-Covid intensive care, according to the Oregon Health Authority.
The jump in cost is because Covid patients spend an average of nearly 17 days in the ICU at OHSU, 10 days longer than the state average, according to the latest available data from April 2020 to March 2021.
“We receive a large number of patients critically ill with Covid-19 and other conditions from around the state and provide the maximum level of care available to help them survive, if we can, which often requires longer lengths of stay and more resources. As a result, charges can be significantly higher than community hospital ICUs,” said Tamara Hargens-Bradley of OHSU communications in an email to the Enterprise.
She said Covid patients that receive ECMO treatment, which circulates the blood through a machine to oxygenate it, stay in the ICU between 20 and 30 days.
Hargens-Bradley said OHSU typically collects around 40% of the cost to treat Covid patients. Of those collections, 40% comes from Medicare, 32% is paid by Medicare, and 28% by insurers.
It’s a similar situation at Salem Hospital, where Covid patients needing intensive care stay an average of 14 days – over twice the average stay of non-Covid patients, according to data provided by the hospital.
“Average charges per day for ICU patients (non-COVID) are comparable to ICU COVID patients; however, the latter are higher in overall charges due to the longer length of stay,” Salem Health spokesperson Lisa Wood wrote in an email to the Enterprise.
At Salem Hospital, Covid ICU charges are an average of $8,585 per day, around $1,500 less than the average charge per day for non-Covid patients. These are the numbers charged before the bill is sent to insurance processing, charity care reductions and self-pay discounts.
Multiplying the average daily charge by the average length of stay, Covid patients who are sent to the ICU incur charges averaging $123,195. That’s 1.7 times higher than an average ICU cost. Those are costs incurred before bills are adjusted for insurance processing, charity care reductions and self-pay discounts, Wood said.
Covid care costs may impact future health insurance rates, said Mark Peterson, spokesperson for the state Department of Consumer and Business Services. That will be determined during the state’s annual rate-setting process.
“There could be long-term costs beyond the in-patient care,” Peterson said. “That would be based on patient cost sharing for the services, not for having a pre-existing condition.”
Providence Health and Services requires more staffing and supplies to care for Covid patients, including ventilators, personal protective equipment and respiratory therapists, said Providence spokesperson Gary Walker.
For all Covid admissions at Salem Hospital, over half of the hospital admissions are those covered by Medicare, followed by 25% paid by insurers and 20% by Medicaid. Only 3% of patients take care of the costs directly.
According to the state health authority, patients with Medicare would be charged their deductible of $1,484.
The state pays the entire bill for patients with Medicaid, and costs vary for patients with private insurance.
Money for Medicare comes from the federal budget although recipients face some copays and deductibles, said Tim Heider of the health authority. Medicaid is 75% federally funded, and the rest is covered by state dollars.
The federal Centers for Medicare and Medicaid Services couldn’t readily provide information at the national or state level about pandemic costs covered under its programs. Agency officials said they would have to conduct a special data analysis to determine average costs and federal totals. Taxpayers provide the bulk of the money for the two programs.
In Oregon, Medicaid is a significant item in Oregon’s budget.
The Oregon Health Plan covers 90% of members through local health plans, and they pay a monthly cost that is not expected to change due to Covid costs, Heider said.
That means the majority of state costs are set regardless of the care provided and won’t be impacted, but about 10% of Oregon Health Plan members receive coverage based on individual medical costs and claims, known as “Open Card,” he said. The federal government pays for a majority of Oregon Health Plan’s costs.
Heider said the health authority doesn’t have current cost information for Covid hospitalizations for Oregon Health Plan members. Last year, such care cost $38 million, including claims from both doctors and hospitals. That was less than 1% of the state’s total health care costs under the Oregon Health Plan.
Nonprofit hospitals such as Salem Hospital will lower patient costs up to 100% depending on the patient’s household income. Those who make less than 300% of the federal poverty level will be eligible for full coverage.
“In some cases, patients could only pay a modest deductible or coinsurance; in others, they could be charged thousands or even tens of thousands of dollars,” OHA said in an email to the Enterprise. “Uninsured patients could be responsible for the entire amount.”

News tip? Contact the Malheur Enterprise by email: [email protected].
EXCELLENCE IN JOURNALISM – Available for $5 a month. Subscribe to the digital service of the Enterprise and get the very best in local journalism. We report with care, attention to accuracy, and an unwavering devotion to fairness. Get the kind of news you’ve been looking for – day in and day out from the Enterprise.